Clinician Wellness Series: Burnout
By Anjana Kundu, MBBS, MD, DA, ABIHM
Dayton Children’s Hospital
Dayton, OH
Introduction
I recently had the opportunity to present a clinician wellness workshop at the SPPM Third Annual Meeting and wanted to share in this article some of the content with everyone.
Lately, we have all read articles, statistics and even books related to physician and clinician burnout. Some articles have gone on to report this as “abuse”. Something that has gained so much attention in the media (alas, a little late), deserves to be discussed amongst a population who not only gets affected personally by it, but may be spreading the outcomes of this affliction unknowingly to others, their patients and perhaps the society at large. The proverb, “physician, heal thyself” rings hollow if, as clinicians committed to helping our patients achieve the best possible health, we are not doing the same for ourselves.
Clinicians are faced with growing challenges in providing high quality, compassionate care with less time and resources for effectively engaging patients as a result of the rush to implement various initiatives, including additional reporting requirements and adoption of new technology such as electronic health records (EHR), coupled with increasing pressure to increase throughput and reduce costs. This resultant “work compression”, where clinicians have to meet the productivity goals in less and less time, compounded with steadily increasing medical complexity in the forms of polymorbidity and increased prevalence of chronic diseases and often psychologically and even physically challenging work environments, is a prime set-up for mental, emotional and physical exhaustion. The risk of burnout among clinicians represents not only personal harm to the clinicians but also a significant threat to system-wide achievement of Tripple Aim goals (better patient experience of care, improved population health, and lower costs). Emerging research shows that clinician stress, fatigue, and burnout are affecting health care systems and the quality of patient care. It is also affecting clinicians' own health and well-being in addition to their job satisfaction.
Burnout is described as a syndrome characterized by an increase in emotional exhaustion, development of depersonalization and a decrease in sense of personal accomplishment. It’s a state of mental, physical and emotional exhaustion caused by excessive and prolonged stress. It is accompanied by feelings of being overwhelmed, unable to meet the constant demands and, over time, results in loss of interest and motivation. With continued stress, burnout may progress to include loss of productivity, poor energy, sense of helplessness, hopelessness, cynicism, pessimism and even resentfulness.
The Maslach Burnout Inventory (MBI) measures the defining characteristics of burnout as follows:
Emotional exhaustion:
Feelings of being emotionally overextended by one’s work, where one is unable to give any more at a psychological level.Depersonalization:
Impersonal and unfeeling response toward the recipient of one’s services, care, treatment or instructions; harboring negative, cynical attitudes and feelings; dehumanizing perceptions of others that can result in viewings one’s customers/recipients as deserving of their troubles and negative occurrences.Personal accomplishment:
Feelings of competence, success and achievement in one’s work with people.
The emotionally exhausted clinician is overwhelmed by work to the point of feeling fatigued, unable to face the demands of the job, and unable to engage with others. The burned out clinician may develop a sense of cynical detachment from work and view people - especially patients - as objects. Fatigue, exhaustion, and detachment coalesce in such a way that clinicians no longer feel effective at work because they have lost a sense of their ability to contribute meaningfully. In the past few years, the growing prevalence of burnout syndrome among health care personnel has gained attention as a potential threat to healthcare quality and patient safety.
Incidence
Although burnout can occur in any occupation, it’s more likely in the human services industry such as healthcare. Thus, clinicians are the prime victims of this affliction.
This year's Medscape survey, echoing other recent national surveys, strongly suggests that burnout among U.S physicians has reached a critical level. In this year's Medscape report, the highest percentages of burnout were reported amongst critical care, urology, and emergency medicine, all at 55%. Family medicine and internal medicine follow closely at 54%. Anesthesiology burnout rates are reported at 51%. In last year's report, the highest percentages of burnout were also in critical care (53%) and emergency medicine (52%). Of note, however, burnout rates for all specialties are higher this year as compared to the previous years. The 2015 survey published in the Mayo Clinic Proceedings compared burnout between 2011 and 2014 and observed an increase in the percentage of physicians reporting at least one burnout symptom, from 45.5% to 54.4%.
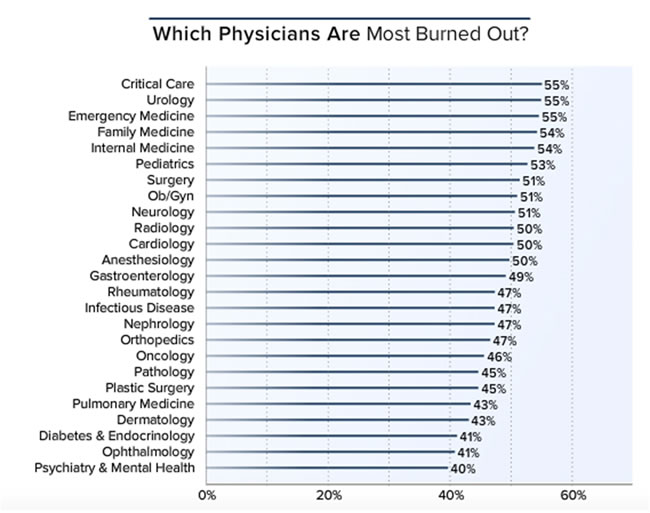
Even amongst the specialties that had a relatively lower incidence of burnout, when asked about how happy they are with their work and work environment, the results are far from reassuring. Dermatologists and ophthalmologists (some of the lowest burnout rates) were the most content, though it is notable that of even these physicians, only one third (39% and 38%, respectively) reported happiness at work. Dermatologists and ophthalmologists were also the happiest at work in the 2014 Medscape survey, but the percentages were much higher (53% and 46%, respectively) compared to this year’s ratings.
Causes
I doubt that this section would come as a surprise to most of you, but often we get so entangled in the day-to-day work that we do not pause to consider the impact of gradually changing elements around us. Burnout is more common as the modern workplace changes to become increasingly economically and psychologically demanding and exhausting. More frequently, economic values are placed ahead of human values. The phenomenon is more likely when there is a mismatch between the nature of the job and the person doing the job. A common indication of this mismatch is work overload. It involves doing too much with too few resources, and going beyond personal limits.
Factors commonly contributing to burnout include work related factors, lifestyle related factors and personality traits.
Work Related Factors:
- Mismatch in workload; unclear or overly demanding job expectations; monotonous or unchallenging work
- Mismatch or lack of control over your work
- Lack of appropriate recognition, rewards or awards
- Loss of a sense of positive connection with others in the workplace
- Working in poorly organized/unorganized or high pressure environment
- Perceived lack of fairness
- Conflict between values
Lifestyle Related Factors:
- Working too much, without time for relaxation, self care or socializing
- Taking on too many responsibilities, without help from others
- Being expected to be too many things for too many people
- Lack of sleep
- Lack of close, supportive relationships
Personality Traits:
- Being a perfectionist
- High achieving, Type A personality
- Need to be in control; reluctance (unwillingness) to delegate
- Pessimistic view (of yourself and of the world)
Presentation of Burnout:
Burnout occurs gradually over an extended period of time and can creep up on you if you’re not paying heed to the warning signs. Although the signs and symptoms are subtle at first and closely resemble stress, they will worsen over time if not addressed early.
Psychologists Herbert Freudenberger and Gail North have postulated that the burnout process can be divided into 12 phases (not necessarily followed sequentially).
- The compulsion to prove oneself
- Working harder
- Neglecting one's needs
- Displacement of conflicts
- Revision of values
- Denial of emerging problems
- Withdrawal
- Obvious behavioral changes
- Depersonalization
- Inner emptiness
- Depression
- Burnout syndrome
However, for practical purposes, I will focus on the factors that signal warning signs that one is heading down the path of burnout. I will also provide differentiation between stress and a frank burnout state.
Warning Signs and Symptoms:
Physical signs and symptoms
- Feeling tired, drained and exhausted most of the time
- Frequent headaches, back pain, increased muscle tension
- Frequent illnesses, low immunity
- Altered appetite
- Altered sleep patterns
Emotional signs and symptoms
- Sense of failure and self-doubt
- Feelings of helplessness, feeling trapped, defeated
- Feeling alone/loneliness
- Feeling of detachment
- Loss of motivation
- Becoming increasingly cynical, pessimistic and with a negative outlook about everything
- Decreased sense of achievement and accomplishment
Behavioral signs and symptoms
- Withdrawal from responsibilities
- Isolation from others
- Taking longer to get things done/procrastination
- Taking out frustrations on others
- Avoiding or skipping work, coming late or leaving early
- Using food, drugs or alcohol to cope
We may consider these as natural effects of our day-to-day work or increased stress periods, but if not heeded, they progress to burnout, at which point we have lost any ability to proactively stop the decline in our physical, emotional and mental states.
Although burnout is a result of persistent, unrelenting and excessive stress, it’s not the same as “too much stress.” Stress usually is a state of excess where it involves too many pressures that demand too much of you, physically and psychologically. It does not, however, deplete you of your imagination, efforts and ability to feel that once you can get it under control, complete this task, and you will feel better. People are usually aware of being under stress.
In contrast, burnout is a state of deficiency. It’s a state of feeling depleted, empty, devoid of motivation and lack of caring for anything or anyone. People experiencing burnout often do not see any hope for positive change in their situations. They are usually unaware of experiencing burnout, akin to experiencing depression.
As the Traditional Chinese medicine practitioners believe, neither excess nor deficiency are good and it is ideal to maintain a balanced state in order to remain healthy.
Prevention and Treatment
The only way to truly prevent and reduce burnout is through a combination of organizational change and education for the individual.
Some organizations have invested in and offer self-care programs. Burnout prevention programs have traditionally focused on cognitive-behavioral therapy (CBT), cognitive restructuring, didactic stress and relaxation. CBT, relaxation techniques (physical and mental), and schedule changes are the best supported techniques for reducing and preventing burnout in a healthcare specific setting.
Individual Initiatives
Being knowledgeable about the risk factors and warning signs of burnout in combination with self awareness and a practice of self-care rituals, including mind/body techniques such as CBT, cognitive restructuring, and relaxation techniques, are powerful personal tools for prevention and management of burnout. Some simple things to incorporate into your routine in order to minimize risks of burnout or to reverse the adverse effects of stress include:
- Begin your day with a relaxing ritual. It does not have to be a lengthy procedure. Instead of jumping out of bed to hit the ground running, you may choose to exercise mindfulness for 3-5 minutes, make yourself a cup of tea, pray, or add a few minutes of stretching or yoga etc.; whatever it is that sets the tone for your day as a mindful activity.
- Adopt healthy eating, exercising, and sleeping habits. Just as there are foods that impact your physical health, foods also have a positive or deleterious effect on your mental health, mood, stress and anxiety state. Choosing foods and drinks that promote physical and mental wellness are optimal. Optimal sleep and a regular activity routine (walking, yoga, Pilates, or other exercise routine) are integral to not only physical but mental health.
- Set boundaries; learn to say no and to delegate. This is not limited to the workplace, but also applies to your personal life. Do not over schedule yourself. There are only 24 hours in a day and a realistic schedule will minimize your stress levels. Moreover, delegation fosters teamwork.
- Take breaks from technology. Schedule time away for technology even if it is for 30 minutes or an hour or, if you wish, an entire day. This allows focusing on the present and what is in front of you, allows tapping into resources not thought of if technology is at your fingertips all the time.
- Nourish your creative side. Incorporate a hobby, a creative activity that is not directly tied into your daily routine or work. Practicing art or music, enjoying it as a recipient, cooking, building, gardening or writing, whatever it might be that you would want to do if you did not have to earn a living, will allow you to nourish your creative side and thus your mental well-being. There is research supporting the role of a hobby in not only one’s heightened well-being, but also in becoming work productivity and leadership development. Again, this does not need to consume you or take so much of your time that it feels like an added stress, but little injections of these activities at some type of regular interval keeps one healthy and productive.
- Learn active strategies for stress management. This will obviously vary from person to person. Some people respond better to active strategies such as physical exercise, while others work well with mental relaxation exercises like CBT, meditation, guided imagery, rituals like prayer, journaling, etc. Whatever it is that works for you, ensure you incorporate that into your life as a regular activity. Minimize the development of stress, before it starts to impact you adversely.
Combining both organizational and individual level activities is without a doubt the most beneficial and successful approach to preventing, reducing and managing burnout symptoms. Therefore, engaging your institution in recognizing and investing their efforts into employee well-being is instrumental in creating a healthy workplace and combating clinician burnout.
For more information or for development of a clinician wellness program, please feel free to contact me at [email protected].


