Long-Term Opioid Use after Orthopedic Surgery Among Children in an Accountable Care Organization
By Emmanuel Alalade, MD, Timothy P. Smith, MD, Dmitry Tumin, PhD, Rebecca Miller, BS, Giorgio Veneziano, MD, David P. Martin, MD, Joseph D. Tobias, MD, Tarun Bhalla, MD, MBA
Department of Anesthesiology & Pain Medicine
Nationwide Children’s Hospital; The Ohio State University
Columbus, Ohio
(Summarized and submitted by Tarun Bhalla, MD, MBA)
Prescribed opioid use for managing post-surgical pain may increase a child’s propensity for long-term opioid use (1). Opioid use after orthopedic surgery is especially concerning, as these procedures are often performed during adolescence, a high-risk age for illicit opioid usage from prescribed medications (2). We retrospectively assessed the influence of procedure type and patient characteristics on long-term opioid use after orthopedic procedures performed in Medicaid-enrolled children and adolescents who were on the acute pain service (APS) at our institution (Nationwide Children's Hospital). Following IRB approval, patients ≤ 18 years of age referred to the APS after orthopedic surgery during the years 2009-2016 were selected for analysis if they were enrolled in Partners for Kids (PFK)., PFK is an Accountable Care Organization (ACO) serving children covered by Medicaid managed care plans in Central and Southeastern Ohio. Patients with recent (<6 months prior to surgery) outpatient opioid use were excluded.
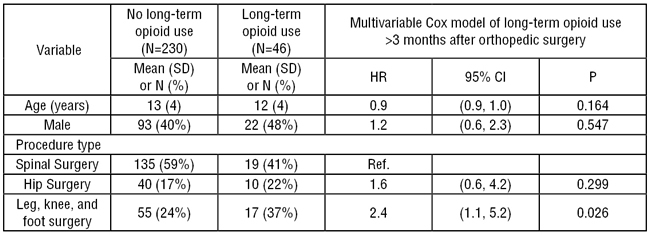
The primary outcome was filling a prescription for opioid medication >3 months after the index procedure, determined from insurance claims data. Patients who dis-enrolled at Accountable Care Organization, or who had subsequent surgery or emergency department visits were not included in follow-up data. Kaplan-Meier plots and Cox proportional hazards regression were used to analyze opioid prescription filling occurring >3 months post-procedure. Independent variables included procedure type, patient age, gender, hospital length of stay (LOS), and procedure year. A total of 276 children were included in the analysis (115/161 male/female, age 12 ± 4 years), with a median follow-up of 16 months (interquartile range [IQR]: 8, 28 months). There were 46 (17%) patients with long-term opioid use (Table 1). Although spine surgery accounted for the majority of the procedures in this cohort, the incidence of long-term opioid use was highest among the 72 patients who had undergone leg, knee, or foot surgery (24% with long-term opioid use; adjusted hazard ratio = 2.4; 95% confidence interval: 1.1, 5.2; p=0.026). No other covariates were associated with an increased incidence of long-term opioid use after orthopedic surgery.
Conclusion: Patients referred to the APS after orthopedic surgery may have a rate of long-term opioid use after discharge. The common practice in our institution is that more complex patients generally require consultation and pain management by the APS. Therefore, these patients may be at an inherent higher risk for developing long-term opioid use and subsequent abuse. Optimizing inpatient management of post-surgical pain may improve chronic pain outcomes of orthopedic surgery and reduce the need for long-term opioid use after discharge, especially for patients undergoing lower extremity procedures.
References:
- Harbaugh CM et al. Pediatrics 2018;141:e20172439.
- Miech R et al. Pediatrics 2015;136:e1169-77.


